Capsular contracture is the development of excessive scar tissue around the breast implants. This guide can give you more information, as well as tips on prevention and treatment.
Breast augmentation remains one of the most popular cosmetic surgeries for women across the world. If you’re considering getting breast implants, you may have heard about capsular contracture. While uncommon, this complication can develop in anyone with breast implants. The good news is that capsular contracture can be managed effectively to preserve both your health and beauty. Here’s a closer look at capsular contracture and a guide to preventing and managing the condition.
Contents
- 1 What Is Capsular Contracture?
- 2 Who Can Get Capsular Contracture?
- 3 How Your Cosmetic Surgeon Minimizes Your Risk of Capsular Contracture
- 4 Does Implant Type Matter?
- 5 Additional Tips
- 6 How Do I Know If I Have Capsular Contracture?
- 7 Can Capsular Contracture Be Treated without Surgery?
- 8 What Happens During Revision Surgery?
- 9 The Bottom Line
What Is Capsular Contracture?
Capsular contracture results from the abnormal hardening of scar tissue surrounding the breast implant, usually initiated by bacterial contamination either during insertion or from the bloodstream. During your breast augmentation healing process, a capsule of scar tissue forms around each implant. This helps preserve the implant and hold it in place. However, in the some instances, the collagen fibers in the scar tissue become overly tightened and cause the capsule to contract. In severe cases, this can distort the shape of the breast and cause soreness and pain.
While capsular contracture can require revision surgery, the condition is completely treatable.
Who Can Get Capsular Contracture?
Technically, anyone who has breast implants can develop capsular contracture. This includes women who have had breast augmentation as well as those who have had implant-based breast reconstruction. The condition may develop as early as 3 months after getting breast augmentation, or as late as 25 years after augmentation.
How Your Cosmetic Surgeon Minimizes Your Risk of Capsular Contracture
While there is no known way to completely prevent capsular contracture from developing, there are some factors that can minimize your chances.
1. Use Proportionate Implants to Your Body
Overly large breast implants tend to stretch and thin the breast tissue, which can lead to a higher incidence of capsular contracture. Large breast implants also have a higher risk of displacement, so selecting the right implant size can help create ideal results in more ways than one.
2. Use an Inframammary Incision
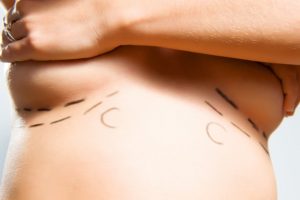
There are three common incision placements for women getting breast augmentation: around the areola (periareolar), through the armpit (transaxillary) and inframammary (in the natural crease under the breast). Studies show that procedures that use the inframammary incision have a significantly lower incidence of capsular contracture. Here’s a look at why:
- The periareolar incision requires insertion of the implant through the milk glands. This means a higher risk of implant contamination, since the milk ducts contain bacteria that may compromise implant sterility. This can lead to the excessive inflammation that initiates capsular contracture.
- The transaxillary incision tends to make use of longer surgical instruments to transport the implant from the armpit to the breast pocket. This distance can also mean more instruments are used and are passed in and out of the incision multiple times, increasing the risk of contamination.
- The inframammary incision offers your cosmetic surgeon optimal access to the breast pocket for precise implant placement. This incision also avoids milk ducts, minimizing risk of contamination. An additional advantage of the inframammary incision is the same incision can be used in the future if you require breast implant revision surgery.
3. Submuscular Placement
Placing the breast implant below the pectoral muscle, known as submuscular placement, limits exposure to bacteria that can contaminate the implant when placed above the muscle, known as subglandular placement. Deciding on breast implant placement means evaluating several factors, most notably, your natural anatomy, and submuscular placement may not be the best choice for everyone. Those who do choose to have their breast implants placed under the pectoral muscles, however, may enjoy a lower likelihood of developing capsular contracture.
4. The Keller Funnel®
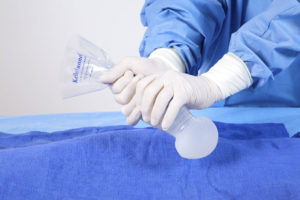
The Keller Funnel® is a device used to insert an implant into the breast pocket using a “no touch” method, meaning your surgeon doesn’t come into direct contact with the implant at any time. Because implants are most likely to become contaminated during insertion, using the Keller Funnel® helps maintain the safest and most sterile environment for your procedure. Studies have demonstrated that the Keller Funnel® can reduce the incidence of capsular contracture by more than 50 percent.
5. The Right Cosmetic Surgeon for the Job
Selecting the best cosmetic surgeon for your breast augmentation is an important process that can determine your final results in many ways. An experienced breast surgeon who stays up-to-date with the latest developments in breast augmentation will have a better understanding of how to create the most beautiful and longest-lasting results.
Surgical technique can be the single most determining factor of your likelihood of developing capsular contracture.
Does Implant Type Matter?
Though there is no full understanding of what causes capsular contracture, the type of breast implant you choose may affect your overall chances of developing the condition.
Saline Implants
Saline implants are smooth and round, and offer many advantages, including easy detection of a leak, lower costs and, in many women, a higher breast profile. However, they may come with a higher risk of capsular contracture.
Silicone Implants
Round implants filled with silicone gel can be smooth or textured. Studies have found that women with silicone implants may have a lower risk than those with saline, though more research is required. In particular, textured breast implants seem to be less likely than smooth implants to develop capsular contracture.
Gummy Bear Implants
Also known as form stable implants, gummy bear implants are also filled with silicone gel. The difference is in the teardrop shape that mimics the natural fall of the breast, making these an excellent choice for subtle and natural-looking results. Gummy bear implants are textured and have a similarly low rate of capsular contracture as round textured silicone implants.
Additional Tips
Some surgeons or medical professionals recommend additional techniques for minimizing your risk of getting capsular contracture:
- Avoid vigorous activity for the first several weeks of your recovery. Strenuous exercise can increase your blood pressure, raise your heart rate and cause bleeding around your new implants.
- While the benefits of massaging the breasts after augmentation are hotly contested, many surgeons and medical professional believe that breast massage may help prevent capsular contracture. Ask your cosmetic surgeon for advice on how to massage the breasts after augmentation.
- Maintain a healthy diet to keep your body nourished with a wide variety of vitamins and minerals.
- Some surgeons recommend taking an antibiotic prophylaxis medication for 1 year or even longer after undergoing major surgery, like a breast augmentation. This can help prevent infection and ensure that you have a healthy recovery.
- Maintain a relationship with your cosmetic surgeon. This may mean checking in with your surgeon every year or couple of years after getting breast implants. While implants can be long-lasting, they are not considered lifetime devices, and keeping an eye on how your results evolve over the years is one of the best ways to manage any complication.
- Finally, one advantage to fat transfer breast augmentation is the ability to enlarge the breasts without implants, negating any risk for capsular contracture.
How Do I Know If I Have Capsular Contracture?
If one or both of your breasts begin to feel unusually firm, tightens into a ball or shifts to a slightly higher position on your chest, you may have capsular contracture. Your breasts may also feel sore to the touch, tight or otherwise uncomfortable. Capsular contracture can start as early as 3 months after surgery.
A physical exam is required for an official diagnosis. A mammogram, MRI or ultrasound may be able to detect the thickened scar tissue, but they are not necessary for diagnosis. If you are diagnosed with capsular contracture, your condition will be classified using the four-grade Baker scale:
Grade I
The breasts feel soft and natural. No treatment is necessary.
Grade II
At this stage, the breast(s) begin to feel a little firmer. For the most part, appearance is still normal. Breast massage may help loosen the collagen fibers in the breast pocket and prevent or delay the condition’s progression.
Grade III
The breast(s) feel noticeably firm and the breast shape may be slightly distorted. You may be able to see the shape of the implant or feel its sides. Revision surgery is often necessary to prevent the progression to Grade IV, though some medications can help soften the breasts.
Grade IV
By this stage, the breast(s) usually feel sore to the touch, hard or even cold. The breast shape is transformed into a tight ball that does not appear natural. Surgery is required to correct.
Can Capsular Contracture Be Treated without Surgery?
Most women experiencing Grade III or Grade IV capsular contracture will require surgery to correct the condition. Depending on the severity, however, you may have some nonsurgical options:
Medications
There are a couple of prescription medications that have demonstrated some effectiveness for preventing the progression of capsular contracture. Depending on the individual case, medications may even soften the tissue enough to completely reverse the condition. These medications consist of leukotriene receptor antagonists, which are commonly used to manage asthma. These medications have shown to soften the scar tissue surrounding the implants. There are two common prescriptions:
- Generic zafirlukast, brand name Accolate, recommended at 20 milligrams twice daily for 90 days
- Generic montelukast, brand name Singulair, recommended at 10 milligrams daily for 90 days
Physical Therapy
Some types of physical therapy may help improve capsular contracture. Physical therapy for capsular contracture can involve a number of different techniques:
- A physical therapist specializing in capsular contracture treatment can manually manipulate the breast tissue in a way that softens and loosens the scar tissue.
- Stretching and breast massage can be done at home with instruction. Do not attempt self-massage before checking with your surgeon and learning the safest and most effective techniques.
- Ultrasonic energy can be applied to the affected breast(s). This treatment is available at certain surgery or therapy centers.
Closed Capsulotomy
Some surgeons use a nonsurgical technique called a closed capsulotomy. This method requires your surgeon to sharply squeeze the affected breast, disrupting and softening the scar tissue around the implant. However, this technique can also result in implant rupture or displacement, and many surgeons do not recommend it. Revision surgery is a much more accepted and effective treatment.
What Happens During Revision Surgery?

If you’ve been diagnosed with capsular contracture, you may require breast implant revision surgery. Most breast implant revision surgeries are performed under general anesthesia. The entire procedure can take anywhere from 2 to 6 hours, depending on your unique case. There are two common methods for resolving capsular contracture with surgery:
1. Open Capsulotomy
In a surgical capsulotomy, your surgeon breaks up the scar tissue using scoring techniques. Some of the scar tissue may also be removed. While capsulotomy may be effective, especially in women with mild to moderate capsular contracture, it does not prevent the condition from recurring.
2. Capsulectomy
During a capsulectomy, your surgeon removes the entire capsule of scar tissue, including the implant, from your breast. He or she then replaces the implant. Because this technique removes the capsule entirely, it is considered the most thorough treatment method.
3. Breast Revision Incisions
If your initial breast augmentation used an inframammary incision, your surgeon will likely be able to use the same incision location for your revision surgery. This means you won’t have any additional scarring.
Women with a different incision may require a new incision placed inside the natural crease below the breast.
The Bottom Line
While only a small minority of women who get breast implants develop capsular contracture, it’s a good idea to take any steps available to you to prevent the complication from developing. Eating healthy, avoiding exercise during your breast augmentation recovery or taking an antibiotic prophylaxis medication can help minimize your chances.
Although it is impossible to completely prevent capsular contracture, you can decrease your chances and keep your peace of mind with a highly skilled cosmetic surgeon.
However, the most important factor by far is your surgeon, as the procedure itself is when the implants are most likely to become contaminated. Choose a surgeon with extensive experience performing breast augmentation with implants and a low incidence of capsular contracture among his or her patients.